
The Deadly Relationship Between Stress and Addiction
Everyone in the world is affected by stress to some extent. The human stress response is a natural reaction to potentially dangerous or damaging situations, whether it be an actual threat to a person’s life or a perceived danger of becoming embarrassed and losing social standing. Stress comes in many different forms and in many different degrees, and everyone has a different ability to cope with stress. They also have different coping mechanisms, some of which may be substance abuse.
The term stress is not a useful objective term to be used as a description of a scientific phenomenon that can be studied. It can neither be defined in objective terms nor can it be measured. It is impossible to objectively measure the amount of stress individuals experience in the same situation because the experience of stress is totally subjective. This results in much of the research involving stress relying on self-report measures of stress from research subjects, and self-report measures are notoriously unreliable.
Unfortunately, self-reporting is all we have to work with. According to the American Psychological Association, the mean stress rating for 2011 was 5.2, on a scale of 1-10, with more Americans reporting their stress levels increasing over time than decreasing.

The endocrinologist Hans Seyle is responsible for many of the common notions of the term stress. Seyle defined stress as a nonspecific response to demands for change. His definition and understanding of how the stress response works is still cited in many texts today despite information indicating that it is probably an insufficient account of what stress is and how it affects the body and mind.
Seyle’s general adaptation syndrome defined the stress response as consisting of three potential stages:
- Alarm: The body and mind experience a stressful condition, and the body becomes mobilized to deal with a stressful situation (flight-or-fight response).
- Resistance: If exposure to the stress continues, the body continues to mobilize resources to deal with the stress.
- Exhaustion: If the person’s stress is not resolved and the stressful situation continues, the system breaks down and the individual becomes vulnerable to different types of diseases and other ailments.

Seyle found that animals exposed to prolonged stressors were more vulnerable to developing different types of diseases. Researchers following up on his ideas suggested that individuals exposed to prolonged periods of stress were also vulnerable to developing certain physical conditions like ulcers and psychological issues like depression.
A more modern-day definition of stress is a general physical and emotional response resulting from the interaction between people and their environments that are perceived to be exceeding or threatening to exceed their adaptive capacities and thus threatening to their wellbeing. There has been much discussion over whether stress is more of an external response that can be measured in chemical changes in the brain, skin reactions, and the arousal of the sympathetic nervous system, or if it’s a psychological interpretation or reaction to a stressor – or both.
Find Fast
Stress and Health
It is generally accepted that experiencing high levels of stress, such as experiencing a traumatic event or being exposed to prolonged periods of stress, is a risk factor for the development of nearly every psychological disorder, including substance use disorders. However, stress can also be result of prolonged exposure to what many would consider positive events, such as planning for a wedding, buying a new house, or adjusting to new living conditions. Therefore, defining exactly what constitutes stress, how to measure stress, and how stress affects different people remains a bit of a conundrum.
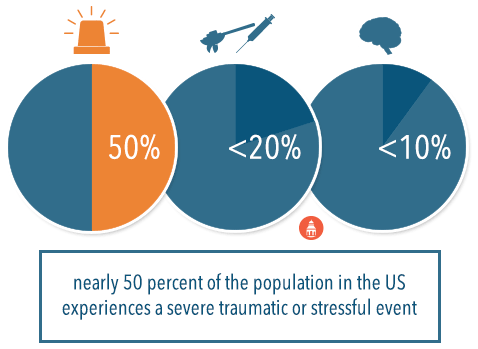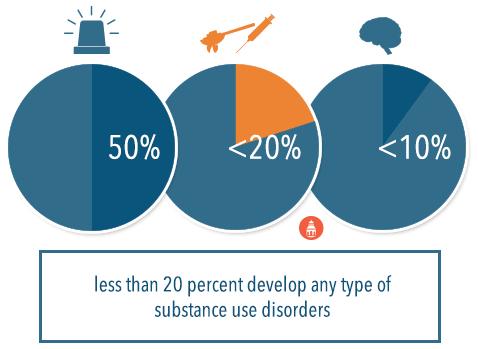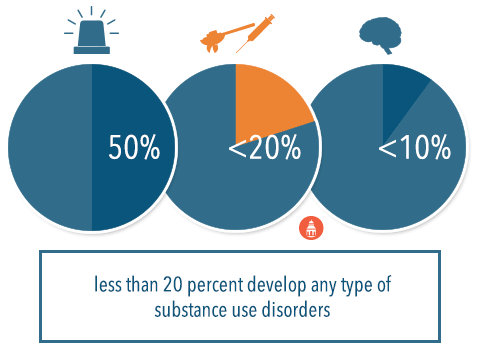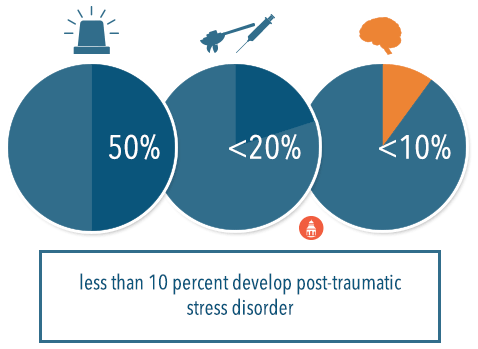
For example, it is estimated that nearly 50 percent of the population in the United States experiences a severe traumatic or stressful event; however, a very small proportion of the population develops post-traumatic stress disorder (less than 10 percent) and few also develop any type of substance use disorders (less than 20 percent of the entire population). Thus, it is inaccurate to say that even experiencing severe levels of stress directly causes substance use disorders or any other health problem, as there are obviously other interacting factors that must be present in these associations.
It’s popular to claim that stress causes or contributes to any number of diseases, from everyday colds to cancer to schizophrenia. This may not be entirely accurate, but there’s still a general consensus among medical scientists that excessive stress can be linked to many health issues, whether that “link” is a partial contributor or something that led to a behavior that caused the problem, such as when “stress eating” contributes to obesity, which contributes to coronary heart disease.
Instead of being a direct causal mechanism for the development of substance use disorders, the experience of either intense or prolonged levels of stress is best described as a risk factor for the development of substance use disorders. According to the World Health Organization, a risk factor is a situation or condition that increases the probability that one will develop a specific type of illness or condition. Either having the risk factor or not having the risk factor cannot guarantee that one will or will not develop some disorder, illness, or other condition; it is only associated with an increased probability that one will develop something.
Stress is also a nonspecific risk factor in that individuals exposed to the same types of stressful conditions may develop a number of different issues or conditions. Other nonspecific risk factors for the development of psychiatric disorders include being abused as a child, experiencing some other form of traumatic event, and having a first-degree relative who is diagnosed with some type of mental health disorder. Individuals who develop substance use disorders most likely have a number of interacting risk factors that contribute to their issues. It is very difficult to generalize which types of risk factors are most likely to result in specific disorders; however, it is known that experiencing high levels of stress or prolonged stress is associated with a number of issues.
Stress and Substance Abuse
The definition of substance abuse depends on the type of substance involved. It’s generally defined as the harmful or hazardous use of an intoxicant, but this, of course, means different things for different people. However, any use of any illicit drug is often considered to be abuse, and use of a prescription medication without medical permission or beyond the prescription’s instructions is also considered drug abuse. According to the Substance Abuse and Mental Health Services Administration (SAMHSA), 24.6 million Americans had used an illicit substance in the month prior to the survey in 2013.
Stress is a well-described risk factor that is associated with a higher vulnerability to the development of substance abuse. There is little evidence to suggest that specific types of stressors can result in specific types of substance use disorders, and attempts to define relationships between the specific types of stressors and specific types of substance abuse inevitably indicate that these types of predictions are not currently possible (and may never be). However, there are several associations that can be made.
First, there is a broad body of research that indicates that adolescents who experience negative life events demonstrate increased levels of substance use disorders. Negative life events, such as parental divorce, high levels of parental conflicts, the loss of a parent, abusive parents, or even low parental support, are associated with higher levels of substance use disorders in adolescents.
Second, more specific evidence has shown a significant association between trauma and maltreatment in childhood and increased rates of substance use disorders in both adolescents and adults; this includes physical and sexual abuse and victimization.
Third, broader evidence indicates that individuals who report experiencing more stressful events over their lifetime or stressful events that are considered to be extreme in their intensity are also associated with higher rates of substance use disorders even when controlling for other risk factors, such as family histories of substance abuse, social economic status, other psychological disorders, etc.
The key in these findings is the term higher rates of substance abuse. Not all individuals who experience extreme stress develop issues, and certainly developing a substance use disorder is not exclusive to people who have experienced stressful events. The mechanisms by which stress and substance abuse are related are not well understood. It is known that both severe stressful events and chronic exposure to stress result in neurobiological changes and that chronic substance abuse also results in neurobiological changes. There are a number of hypotheses as to how these factors interact:
- The very popular self-medication hypothesis suggests that individuals who experience chronic levels of stress or extreme stressful events use drugs and alcohol to help them deal with the unpleasant experience of stress. While there is some validity to this notion, it should also be noted that a small proportion of individuals who admit to using drugs and alcohol to cope with stressful experiences develop substance use disorders. In individuals who develop substance use disorders, their substance abuse does not wax and wane in accordance with their stressful experiences. Thus, while some individuals may self-medicate with drugs and alcohol, this explanation cannot be used as an overall causal explanation for the relationship between stress and substance abuse. Research suggests that this may happen, but as an overall explanation, it falls short of explaining the relationship.
- It is also observed that individuals with all types of psychological disorders have higher rates of substance abuse – up to 50 percent according to the National Alliance on Mental Illness – and report higher levels of stress than individuals who are not diagnosed with these disorders. One explanation is that individuals who are prone to developing any type of psychological disorder are also more vulnerable to developing substance use disorders due to a number of shared risk factors, such as similar neurobiological pathways, genetic associations, environmental experiences, etc. Thus, individuals prone to the development of any form of mental illness are also more vulnerable to the development of substance abuse.
- An individual’s style of interpreting the world and events appears to have a profound influence on their experience of perceived stressors and their vulnerability to developing substance use disorders or other mental health disorders. Individuals who generally view their experiences and actions as being within their sphere of control, and their feelings and attitudes as being subject to change, are less likely to suffer ill effects from stress and to develop substance use disorders. These types of attitudes and perceptions are largely learned, and they are also based on experience. Thus, belief systems and attitudes can be changed and altered for better or worse. Part of the saliency of stress as a potential contributor to the development of substance use disorders or any other mental health disorder is dependent on individual perceptions regarding control over their reactions to the events in their lives. Individuals who perceive they have more control will tend to experience stressful events as less threatening and less stressful. These individuals should be at decreased risk to develop substance use disorders as well. Research supports this notion.
Addiction

Substance abuse may begin partially because of stress, but a substance use disorder – commonly referred to as an addiction – is more complex. Although substance abuse can alleviate stress, an addiction is characterized by chronic drug-seeking and use in spite of negative consequences. At the point of addiction, substance use is a constant source of stress. An addicted individual is often constantly preoccupied with how and when the drug will be obtained next. Negative consequences like loss of friends, family disapproval, loss of a job, and financial and legal troubles are all significant sources of stress, yet instead of trying to avoid or resolve these problems to lesson stress, an addicted person is compelled to continue.
This is why addiction is currently defined as a chronic, relapsing brain disease or mental illness. According to the National Institute on Drug Abuse, this disease affected around 23.5 million Americans in 2009. People who are sensitive to stress are actually more likely to avoid substance use than become addicted to a substance due to the risks involved. Addicted persons continue using because of a psychological and physical need for the drug and the reinforcement of the brain’s pleasure center to the drug-seeking behavior.
That’s not to say that stress doesn’t play a role in continuing addiction. Many addicted individuals avoid or put off attempting to quit because of the anticipated extreme discomfort of withdrawal – a medical condition characterized by physical and psychological symptoms caused by the sudden lack of a substance that a person’s brain has grown accustomed to.
Some of those fears are more than warranted. Detoxing from a severe substance use disorder can be dangerous with certain types of substances, particularly alcohol and benzodiazepine anti-anxiety medications. Fortunately, there are plenty of treatment options to get addicted persons safely and comfortably through withdrawal that can also address any stressors in one’s life that may be contributing to the disorder.
Call Now (619) 577-4483
Treatment Options
Whether or not stress is a contributor to a substance use disorder, an addicted person needs to enter treatment as soon as possible for detoxification and rehabilitation to avoid a myriad of potential health problems, some of which can be permanent. Although it’s essential to address potential stressors and co-occurring mental illnesses during the treatment process, it’s much easier to address these factors when the addicted person is off the drug.
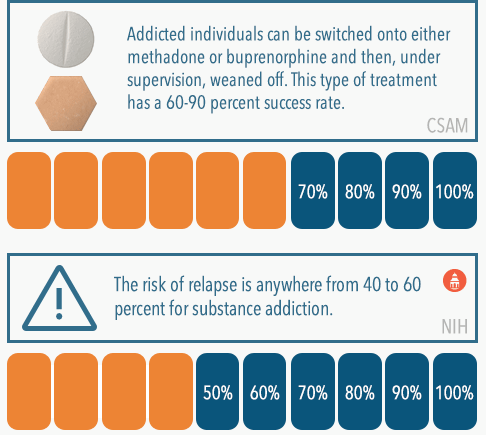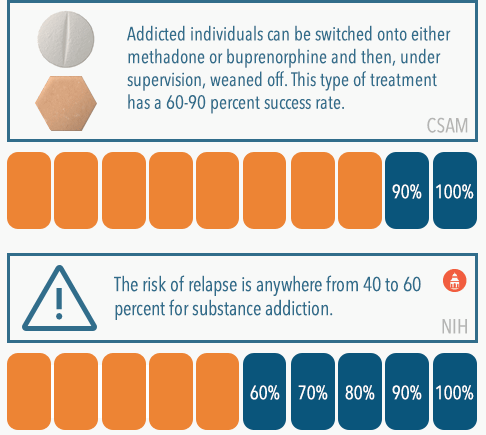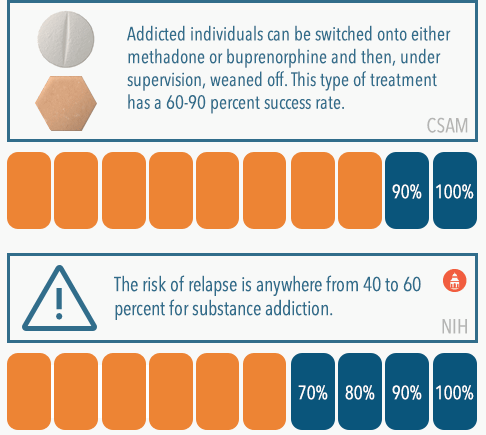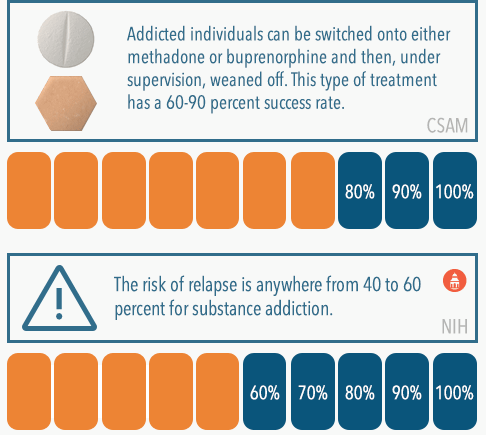
The stress of facing withdrawal can be alleviated by a couple different treatment options. For addiction to opioids such as heroin, Vicodin, and fentanyl, there are medications that can be used to directly treat the disorder. Methadone and buprenorphine are both medications that have been approved for use to treat opioid addiction. As opioids themselves, they reduce or eliminate cravings and withdrawal symptoms. They’re also much less powerful than commonly abused opioids – the high they produce is nothing to someone with a high tolerance to this class of drug; therefore, there is little temptation to abuse them. Addicted persons can be switched onto either methadone or buprenorphine and then, under the supervision of a medical professional, weaned off the medication. According to the California Society of Addiction Medicine, this type of treatment with methadone has a 60-90 percent success rate.
Medically assisted detox is also an option for those who need to quit taking a substance all at once. This common program allows addicted individuals to stay in a hospital setting for the duration of the worst withdrawal symptoms – typically a few days to a week or more. Doctors remain on site to monitor clients for any dangerous symptoms and immediately treat any of the uncomfortable ones. The goal of medically assisted detox is to ensure that clients remain as comfortable as possible during the process. Signs of distress are taken as signs that the treatment is not ideal.
Because stress and co-occurring mental illnesses are so common in people with substance use disorders, it’s important to participate in a rehabilitation program after detox is complete or during the weaning process. Rehab typically includes a psychological screening during the intake process to check for serious stressors, past trauma, and co-occurring illness. Individual and/or group therapy is also common to help clients get to the root of any issues that could be contributing to substance abuse. There are also a variety of workshops provided that can help addicted persons learn to manage or lessen stress in their lives or address the problem indirectly by teaching job skills, interview skills, communication skills, etc.
Treatment for trauma and stress-based disorders often includes an element of cognitive restructuring from therapies, such as Cognitive Behavioral Therapy and mindfulness therapy. These cognitive restructuring techniques allow the individual to more objectively assess their responses to stressful events, objectively confront and cope with issues related to anxiety and fear, and learn to control their responses to perceived stress. When individuals have a better developed sense of control over themselves and their reactions to environmental stressors, they tend to perceive stressful events as less threatening. Likewise, these individuals are less apt to develop future issues with substance use disorders.
After rehab, it’s generally recommended for recovering individuals to continue treatment in some form, often referred to as aftercare. Continuing to attend therapy and/or addiction support group meetings can be very helpful in keeping stress levels down, reducing the risk of relapse, which is anywhere from 40 to 60 percent for substance addiction. Spiking stress levels are often identified as common triggers to use, meaning that they can cause a recovering individual to experience a sudden and intense craving that often leads to a return to substance abuse.
Conclusions
 There is an obvious relationship between the experience of stress and the development of substance use disorders; however, the relationship between these entities is very complicated. Specific predictions are difficult to make regarding what types of stressors will lead to the development of substance abuse.
There is an obvious relationship between the experience of stress and the development of substance use disorders; however, the relationship between these entities is very complicated. Specific predictions are difficult to make regarding what types of stressors will lead to the development of substance abuse.
The experience of stress is highly subjective in nature, and there can be no claim that stress causes the development of a substance use disorder. Because stress is a risk factor for the development of substance use disorders and its perception is based on subjective interpretations, assisting vulnerable individuals who are exposed to stressful events to learn stress management techniques should reduce their risk for the development of substance use disorders. Those who have already developed an addiction can still maintain a healthy life after treatment via stress management skills as well.
