
As the most populated state in America, California has not been immune to the effects of the opioid epidemic that has swept across the country. From the rich suburbs to the desert towns, Californian doctors are struggling to control a wave of overdoses that have been fueled by a black market of prescription medication and heroin. Statistics on opioid use in California reveal a troubling trend, but the medical community is rallying to turn a dire situation around.
Reaching California’s Shores
The New York Times calls it a “ripple” of drug overdose deaths that has spread across the country. It had its beginnings on the East Coast, in places like New Jersey (where many pharmaceutical companies have set up shop) and Appalachia, where blue collar workers are pressured to work through their on-the-job injuries in declining industries. But due to drug smuggling, the dark web, and massive pharmaceutical lobbies, the abuse and diversion of powerful prescription painkillers have made their way to California, bringing (and reviving) the heroin trade as well.[1]
Bakersfield.com writes of how the opioid problem “is one of the worst healthcare crisis California has ever seen.” Even as the epidemic wreaks havoc on a national scale, California is being hit hard; hospitals in the state treat one heroin or prescription opioid overdose every 45 minutes. In 2014, California lost 4,521 of its residents to overdoses, the largest number of any state in America. In Bakersfield’s Kern County, 131 people lost their lives to opioids between 2011 and 201, and a further 1,112 were hospitalized.[2]

In 2013, hospitals in the Golden State saw more than 11,500 patients who were admitted for heroin or other opioid overdoses, an increase of more than 50 percent since 2006. The Sacramento Bee equates that to one overdose every 45 minutes.[3]
The problem is worse in the state’s rural regions. Hospitals in Shasta County (the 31st most populous of California’s 58 counties) saw more than 1,100 people overdose between 2006 and 2013, which is roughly eight overdoses per 10,000 people. That amount is three times that of the state’s average.
Similarly, other counties, like Sacramento, Placer, and El Dorado, have opioid overdose rates that are higher than the overall Californian average; only Yolo County came in with overdose rates that were lower.
Overdoses that resulted in emergency room visits and hospitalizations were also up, the Office of Statewide Health Planning and Development reported, between 2006 and 2013.
More than Any Other Medication
California’s distance from the epicenter of the opioid epidemic has given its doctors and medical associations time to respond, but a lot of damage has been done. Business Insurance writes that the rate of painkiller consumption among injured workers has dropped in the last few years, but opioids nonetheless make up more than 25 percent of all prescriptions that are filled in California.[4]
Medical provider networks and independent medical review processes have helped reduce the number of opioid prescriptions given to patients and the dosages of those prescriptions, according to the California Workers’ Compensation Institute (CWCI).
Yet, the opioid legacy remains. CWCI laments that opioids are the “single largest category of medications prescribed to injured workers,” a conclusion it drew from looking at data from almost 11 million Californian workers who were given opioid prescriptions as a result of workplace injuries between 2005 and 2014. Opioids beat out anti-inflammatory drugs, ulcer drugs, antidepressants, dermatologicals, anticonvulsants, and ulcer drugs, in terms of how often they were prescribed.
But there is a slowdown, and one reason may be cost. The average payment per opioid prescription went up by 85 percent between 2005 and 2014; other prescriptions, by contrast, increased only 39 percent.
California’s CURES
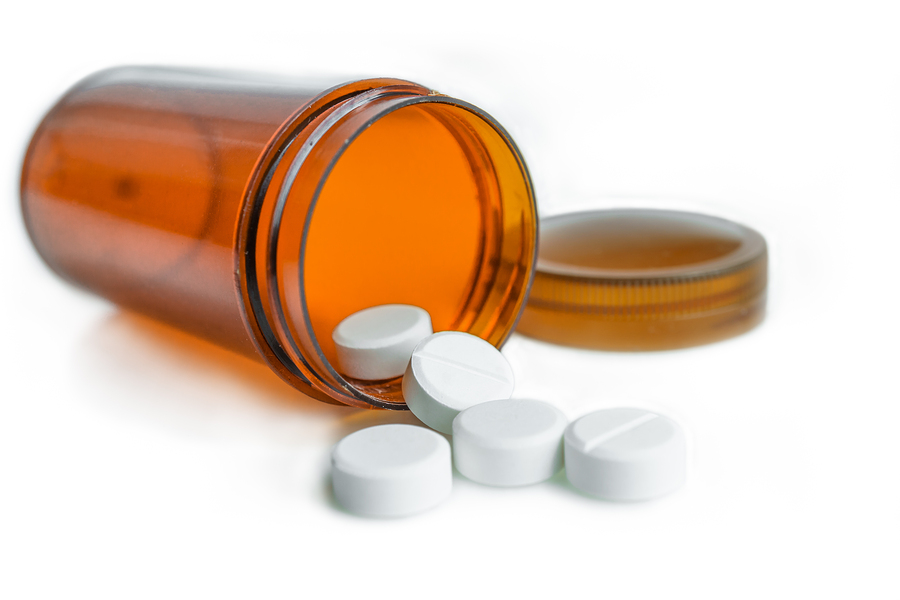 The Los Angeles Times writes of some efforts to turn back the tide. In the face of rising deaths from opioid overdoses (which have risen steadily in the last decade), the Controlled Substance Utilization Review and Evaluation System, or CURES, was created by Californian lawmakers to impose some controls over the rampant overprescription of narcotic painkillers. Pharmacists are required to enter into the database any customers who receive potentially addictive drugs; doctors, however, are not required to check the CURES database before they write a prescription.[5]
The Los Angeles Times writes of some efforts to turn back the tide. In the face of rising deaths from opioid overdoses (which have risen steadily in the last decade), the Controlled Substance Utilization Review and Evaluation System, or CURES, was created by Californian lawmakers to impose some controls over the rampant overprescription of narcotic painkillers. Pharmacists are required to enter into the database any customers who receive potentially addictive drugs; doctors, however, are not required to check the CURES database before they write a prescription.[5]
A 2013 survey by the Substance Abuse and Mental Health Services Administration found that 66 percent of the people who abuse prescription medication hadn’t even received the drugs from their doctor; they either “borrowed” the pills from a friend or family member, stole them, or bought them online.[6] Such people would not be in the CURES database, but doctors and pharmacists could nonetheless use the program to identify so-called “doctor shoppers”: people who go from doctor to doctor to procure prescriptions, and thus cut off one way controlled medication is diverted from its intended use.
Loosening the Rules
But the battle to control opioid use in California will not be easily won. In the spring of 2016, lawmakers – and President Barack Obama – signed the Ensuring Patient Access and Effective Drug Enforcement Act of 2016, which the Los Angeles Times writes was received with “little attention and virtually no public opposition.” The Times warns that the act hinders government in taking action against the pharmaceutical industry itself: Companies that do not report suspicious orders of addictive (and potentially deadly) drugs are allowed to submit a plan of action to the Drug Enforcement Agency, which allows the companies to postpone, or even nullify, any government action taken against them. The act also makes it more difficult for the DEA to temporarily suspend the licenses of pharmaceutical companies involved with the manufacture and distribution of such drugs.[7]
“Amid the opioid epidemic,” the Times put it, “[the] rules for drug companies are loosened.”
Supporters, like pharmacy industry groups, praise the law because it keeps medication available for legitimate purposes and the patients who need them, and further encourages cooperation between the pharmaceutical industry and the government (especially law enforcement).[8] Scientific American warns that regulating the prescription of painkillers too tightly will deprive needy patients of powerful medications that can actually help them.[9]
Critics, however, point out that such companies have much greater leeway (even flexibility) in detecting and reporting diversionary drug flow. One such critic was Joseph Rannazzisi, the DEA official in charge of the regulation of pharmaceutical firms. Rannazzisi resigned his post in late 2015, because he felt that that the act “was misguided and would worsen the epidemic.” Congressional lawmakers disagreed, and after a “bitter dispute,” Rannazzisi walked away from the agency.
Pill Mills in Los Angeles
California has a very good reason to be skeptical of a law that lightens restrictions on pharmaceutical companies. In a single week in September 2008, a pill mill in MacArthur Park in Los Angeles placed orders for 1,500 oxycodone painkillers, sold as OxyContin by Purdue Pharma – two of the most infamous names in the opioid crisis, and largely blamed for the start of the overprescription trend.[10] That order – 1,5000 in a week – is more than legitimate pharmacies sold in a month. The next month, the doctor prescribed 11,000 pills; by December, she gave out more than 73,000, at a street value of almost $6 million.
In Connecticut, Purdue Pharma tracked the prescriptions, with a sales manager discovering that the MacArthur Park pharmacy was in cahoots with another pill mill out of Huntington Park. She asked her supervisors if Purdue should inform the DEA of what she called “an organized drug ring,” but Purdue quashed the inquiry and kept silent about the issue for several years, until the clinic was shut down and its leaders charged. When that finally happened, over 1 million OxyContin pills had found their way into the hands of organized crime rings and gangs.[11]
The Los Angeles Times found that Purdue Pharma had “extensive evidence” that showed OxyContin was being illegally distributed in the two sites in California, but opted not to share the information with law enforcement. A former executive for the company told the Times that even when the company knew that pharmacists were selling pills to drug dealers, Purdue “did not stop supplying distributors selling to those stores.”
One of the rings that was on Purdue’s silent radar was in Monterey Park, represented by Judy Chu. The Center for Responsive Politics reports that Chu was a co-sponsor of the Ensuring Patient Access and Effective Drug Enforcement Act, and
has received contributions of over $31,000 from the pharmaceutical industry.
In a statement, Chu said she was “deeply concerned” about Purdue’s decision to not report diversionary practices to the government, but stood by her support for the new law, claiming that it would lead to “the guidance needed to end the prescription drug epidemic.”
Not all of California’s politicians are so amenable to the overtures of the pharmaceutical industry in their state. Two of the state’s congressmen, both members of the House Oversight and Government Reform Committee, called for a formal investigation of opioid manufacturers.
One of them, Mark DeSaulnier of Concord, is well aware of the prescription medication problem in California. As a senator in 2013, he was part of a law that improved the prescription monitoring program, which helped authorities identify and go after patients who shopped for doctors and physicians who prescribed beyond safety regulations. DaSaulnier told the Los Angeles Times that the reason behind his support for a congressional investigation was because Purdue Pharma seemed to be getting away with how it withheld information about pharmacists in collusion with criminals in California.[12]
Fentanyl
 OxyContin was the drug at the heart of the opioid epidemic, but other medications – most of them still based on the same chemical compounds as heroin – have grown the problem. One such medication is fentanyl, a synthetic opioid that is nearly 50 times more potent than heroin and over a hundred times more powerful than morphine. In Russia, special forces used a derivative of fentanyl to kill 40 terrorists during a hostage incident in 2002.
OxyContin was the drug at the heart of the opioid epidemic, but other medications – most of them still based on the same chemical compounds as heroin – have grown the problem. One such medication is fentanyl, a synthetic opioid that is nearly 50 times more potent than heroin and over a hundred times more powerful than morphine. In Russia, special forces used a derivative of fentanyl to kill 40 terrorists during a hostage incident in 2002.
In California, fentanyl was implicated in 51 overdoses, in a matter of weeks in the spring of 2016. Eleven of those cases were fatal, all in less than a month. The first sign of trouble came in March 2016, when in two days, emergency rooms in Sacramento County reported a dozen overdoses; within a week, the number went up to 35.[13] Doctors at UC Davis Medical Center were confounded by overdose signs that were far beyond the toxicity normally associated with heroin,
A report issued by the California Senate Committee Public Safety observed that “users are often unaware that they are using fentanyl,” a drug so strong that a dose equivalent to just a few grains of salt can kill. As a result of this, people who abuse fentanyl (whether recreationally or misguidedly) tend to take large amounts of the drug at a time.
Call Now (619) 577-4483
Only a Matter of Time
Complicating the problem is the fact that fentanyl is easy to produce, giving organized crime rings and Central and South American drug cartels an easy substitute for oxycodone or even heroin itself. At only $5 a pill, fentanyl is the newest wave of the opioid epidemic that has reached California. Like the victims of the crisis in towns and neighborhoods across America, the Californians who overdosed on fentanyl represented a crisscross of demographics: They were between the ages of 18 and 59, and evenly split by gender.
Los Angeles County saw fentanyl overdoses rise from 42 in 2011 to 62 in 2014. The spike is not as severe as that found on the East Coast, but the medical director of the LA County Department of Public Health’s Office of Substance Abuse Prevention and Control is nonetheless pessimistic. Speaking to the Los Angeles Times, Dr. Gary Tsai worries that “it’s only a matter of time” until Los Angeles County – at more than 10 million residents, the most populous county in the United States – will fall under the sway of the prescription opioid epidemic.[14]
The director of a Sacramento-area needle exchange program says that her organization has been readying itself for the problems associated with fentanyl abuse. Users are at risk for lowered blood pressure, breathing, and heart rate, to the point of the body shutting down entirely, much quicker and more completely than with other opioids.
Heroin by the Kilo
But identifying fentanyl abuse isn’t always easy. Sacramento County health officials have noted that a number of the fentanyl overdose cases have occurred after people bought what they believed to be a less potent opiate called Norco. In reality, however, they were purchasing fentanyl, perhaps the deadliest of synthetic opioids. The Los Angeles Times reports that the disguised fentanyl has made its way as north as the Bay Area. A special agent for the DEA pointed out that the cases of Norco poisoning in Sacramento County and the Bay Area happened around the same time, leading to speculation that one drug cartel could have supplied the medication to both regions.[15]
The co-director of the Johns Hopkins Center for Drug Safety and Effectiveness identifies Sacramento County’s problem as “just another face of the opioid epidemic” that the rest of the country, and California itself, has been struggling with. In Sacramento County, methamphetamines have been displaced by heroin as the drug atop the mountain. A sergeant at the Sacramento County sheriff’s major narcotics impact division tells the Los Angeles Times that 15 years ago seizures of few ounces of heroin by his department were rare; today, however, police find heroin by the kilo.
California’s proximity to the Mexican border makes it a target destination for Mexican cartels, which buy fentanyl produced in China, and then use their standard methods of delivering the product to the United States. One such method involved an underground tunnel that stretched for nearly a half-mile, the largest one yet found by law enforcement agencies. The northern end of the tunnel made ground between the Otay Mesa Port of Entry and the California Highway Patrol’s border base.[16]
When federal agents busted that tunnel in April 2016, they found that it was used mostly for transporting cocaine and marijuana, but fentanyl has been a popular commodity for the cartels. In 2014, DEA agents found 26 pounds of fentanyl in a Los Angeles stash house. More recently, in July 2016, a woman was arrested by federal agents on the charge of trafficking fentanyl into Sacramento County. If convicted, she could be sentenced to a 20-year prison term.[17]
Stopping the Opioid Epidemic
 Opioid trafficking in California is a big operation, whether conducted by drug cartels or individual criminals. But whoever is behind it, the victims are always the same: innocent people, some of whom have become desperate for opioids for their pain; others who misguidedly think that by getting high off legal substances, they can’t be doing themselves too much damage. Writing in the San Francisco Chronicle, a doctor says that it will require a concentrated effort to stop the trend of rampant opioid consumption.
Opioid trafficking in California is a big operation, whether conducted by drug cartels or individual criminals. But whoever is behind it, the victims are always the same: innocent people, some of whom have become desperate for opioids for their pain; others who misguidedly think that by getting high off legal substances, they can’t be doing themselves too much damage. Writing in the San Francisco Chronicle, a doctor says that it will require a concentrated effort to stop the trend of rampant opioid consumption.
Part of the problem comes from the medical community itself. In the mid-1990s, pharmaceutical manufacturers (like Purdue Pharma) embarked on a massive campaign to “liberalize the approach to pain management,” and certain doctors in the California Blue Shield network have showed “a casual approach to opioid prescribing.”
Blue Shield California has launched a program that has targeted the end of 2018 as the time by which the number of opioids prescribed to patients should drop by 50 percent. The plan is to help patients who are on high dosages to shift to reduced, safer dosages, and to provide patients who haven’t been prescribed opioids with alternatives. One example of an alternative might be medicinal marijuana, which was a suggestion put forward by a study out of the University of Georgia. In the 17 states (and the District of Columbia) that allow cannabis to be prescribed and dispensed for legitimate medical purposes, more than $165 million were saved on prescription drugs in 2013. The study found that there was a significantly reduced demand for opiates and other painkillers, all of which are potentially habit-forming.[18]
The California Health Care Foundation is taking similar steps to curb the trend of opioid use (and abuse), such as investigating other treatment options, partnering with competing healthcare providers, and working closely with the Justice Department on improving the prescription medication database and getting more doctors to use it.[19]
Behind the Curve
The New Yorker writes that California has long been the country’s political bellwether; other states, and even the federal government, will usually follow in the Golden State’s footsteps when it comes to passing laws.[20] This is a badge of pride for most Californians, says the Sacramento Bee, because it means their state is ahead of the national curve.[21]
But California has fallen behind other states when it comes to tracking and curbing the abuse of prescription opioids. Only 34 percent of the state’s medical professionals licensed to prescribe or give out controlled substances are registered to use the government’s online database to monitor the flow of prescription drugs. While Arizona and New Jersey – which has been hit particularly hard by the epidemic – actively require doctors and pharmacists to check their respective state databases before prescribing medication (a similar program in New York led to opioid prescriptions dropping by 9 percent and doctor shopping plunging by almost 75 percent), the California Medical Association has opposed the local measure, on the grounds of any such measure “[legislating] the practice of medicine.” Doctors should have the right to prescribe the medication they want to patients, without the pressure to check names against a database.

The opposition is at odds with the California Chamber of Commerce, police groups, consumer advocates, insurance companies, lawyers, and unions alike, all of which support the implementation of a drug monitoring program.[22]
Paying the Price
For now, opioids remain the most prescribed medication in California, writes Business Insurance.[23] Even as trends show that such drugs are being prescribed less, they remain the dominant painkillers in workers’ compensation programs, both in California and across the country.[24]
In August 2016, to coincide with International Overdose Awareness Day (August 31st), the Obama administration announced the allocation of $53 million in grants, to help states implement policies to fight the opioid epidemic. The announcement came with a warning that even $53 million is a “fraction of the funding needed” to fully combat the crisis. California stands to receive $78 million over a two-year period.[25]
Some of that money will be sent to drug court programs, like one in Sacramento County, where parents who complete mandated addiction treatment will be reunited with their children. A social worker told NPR that what the county is doing is a radical difference to how the judicial system used to handle cases of drug abuse: sending people to court and blaming them for their problems.[26]
Now, by giving people the tools they need to recover – “support, medication-assisted treatment, and tough love” – there is the growing hope that treating opioid abuse (which has been blamed in some of the 80 percent of cases where Child Protective Services remove dependents from homes due to substance abuse) can reunite families.[27]
There is cause for cautious optimism: The director of Sacramento’s Health and Human Services Department praised the drug court program, saying that this line of rehabilitation provides “the most effective motivation” she has ever seen, to help people overcome their addiction.
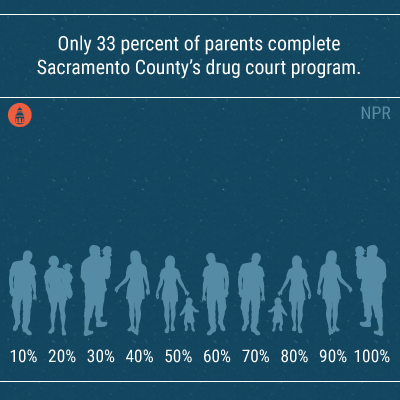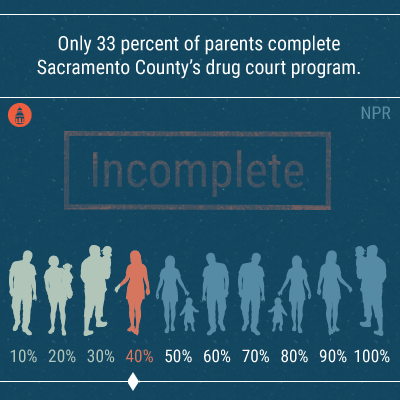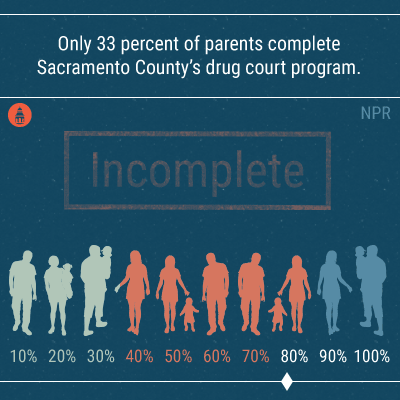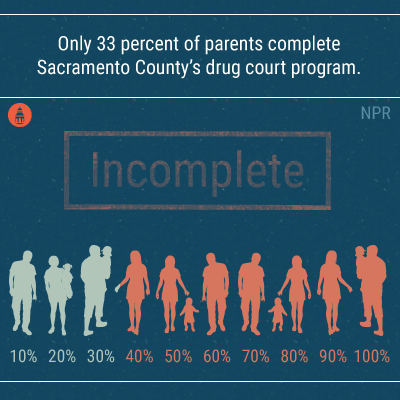
But, as with the state overall, much work remains to be done. The social worker told NPR that only 33 percent of parents (either single or still with their partner) complete Sacramento County’s drug court program. For many people, the physical rush of a drug hit is too difficult to overcome. “If these parents aren’t successful [in graduating from the program],” he says, “it’s the kids who pay the price.”
Citations
[1] “How the Epidemic of Drug Overdose Deaths Ripples Across America.” (January 2016). The New York TImes. Accessed August 30, 2016.
[2] “Opioid Epidemic Facing Our State Is Critically Grim.” (June 2016). Bakersfield.com. Accessed August 30, 2016.
[3] “See Where California’s Heroin, Opioid Problems Are Worst.” (August 2015). The Sacramento Bee. Accessed August 30, 2016.
[4] “Opioid Prescriptions Down In California, But More Effort Needed.” (May 2016). Business Insurance. Accessed August 30, 2016.
[5] “CURES Bill Could Make A Dent In California Prescription Drug Abuse.” (May 2015). Los Angeles Times. Accessed August 30, 2016.
[6] “Results from the 2013 National Survey on Drug Use and Health: Summary of National Findings.” (September 2014). Substance Abuse and Mental Health Services Administration. Accessed August 30, 2016.
[7] “Amid Opioid Epidemic, Rules For Drug Companies Are Loosened.” (July 2016). Los Angeles Times. Accessed August 30, 2016.
[8] “Obama Signs Patient Access And Effective Drug Enforcement Act.” (April 2016). Chain Drug Review. Accessed August 30, 2016.
[9] “Opioid Addiction Is a Huge Problem, but Pain Prescriptions Are Not the Cause.” (May 2016). Scientific American. Accessed August 30, 2016.
[10] “How The American Opiate Epidemic Was Started By One Pharmaceutical Company.” (March 2015). The Week. Accessed August 30, 2016.
[11] “More Than 1 Million OxyContin Pills Ended Up In The Hands Of Criminals And Addicts. What The Drugmaker Knew.” (July 2016). Los Angeles Times. Accessed August 30, 2016.
[12] “California Representatives Call For Congressional Investigation Into Purdue Pharma And Other Opioid Makers.” (August 2016). Los Angeles Times. Accessed August 30, 2016.
[13] “Fentanyl: The Drug That’s Ravaging Sacramento.” (April 2016). Pacific Standard. Accessed August 30, 2016.
[14] “Death Toll Rises To 9 In Suspected Fentanyl Overdoses In Northern California.” (April 2016). Los Angeles Times. Accessed August 31, 2016.
[15] “‘Norco’ Fentanyl Overdose Deaths Rise To 14; Problem Spreads To Bay Area.” (April 2016). Los Angeles Times. Accessed August 31, 2016.
[16] “U.S. Border Agents Seize Longest Mexico-California Drug Tunnel Yet.” (April 2016). Reuters. Accessed August 31, 2016.
[17] “Woman Accused Of Trafficking Fentanyl To Sacramento County Following Wave Of Overdose Deaths.” (July 2016). Los Angeles Times. Accessed August 31, 2016.
[18] “Legalizing Medical Marijuana Decreases Use of Opiates: Study.” (July 2016). TeleSUR. Accessed August 31, 2016.
[19] “It Takes The Efforts Of Us All To End The Opioid Epidemic.” (July 2016). San Francisco Chronicle. Accessed August 31, 2016.
[20] “What California Can Teach Other States About Climate Change.” (April 2015). The New Yorker. Accessed August 31, 2016.
[21] “California’s Best Tool For Ending Opioid Abuse Is Underused.” (March 2016). Sacramento Bee. Accessed August 31, 2016.
[22] “Father Fights Opioid Addiction, To Save The Next Father’s Son.” (February 2016). Sacramento Bee. Accessed August 31, 2016.
[23] “Opioids Remain Most Prescribed Pain Medication In California.” (May 2016). Business Insurance. Accessed August 31, 2016.
[24] “Opioids Still Top Prescription in CA’s WC, Even After Recent Declines.” (May 2016). WCInsights. Accessed August 31, 2016.
[25] “Obama Administration Announces Grants To Fight Opioid Epidemic, Urging More Funds For Treatment.” (August 2016). Los Angeles Times. Accessed August 31, 2016.
[26] “California Court Helps Kids By Healing Parents’ Addictions.” (August 2016). NPR. Accessed August 31, 2016.
[27] “Heroin, Opioid Abuse Put Extra Strain On U.S. Foster Care System.” (October 2015). NPR. Accessed August 31, 2016.
